Schamberg disease represents the most common type of pigmented purpuric dermatoses (PPDs), a chronic, benign, cutaneous eruptions characterized by petechiae, purpura, and increased skin pigmentation (brown, red, or yellow patchy).
In Summary:
Schamberg disease is a skin ailment that produces pigmentation of the lower limbs. It mainly affects the lower limbs and very rarely elsewhere, and is the most common type of pigmented purpuric dermatoses (PPDs): a chronic, benign, cutaneous eruption characterized by petechiae, purpura, and increased skin pigmentation.
[ninja_tables id=”73418″]
The PPDs are grouped into five clinical entities: Schamberg’s purpura, Majocchi purpura, lichen aureus, Gougerot-Blum purpura and, eczematid-like purpura of Doucas and Kapetanakis.
Schamberg disease (SD) has also been called: progressive pigmentary dermatosis of Schamberg, purpura pigmentosa progressive, and Schamberg’s purpura. It is commonly seen in males and mainly affects the tibial regions, and could involve thighs, buttocks, trunk, or upper extremities.
This article focuses on this schamberg disease; What causes it? What are its symptoms? How can it be prevented? What are its treatments?
Let’s proceed to find out more.
What is Schamberg Disease (SD)?
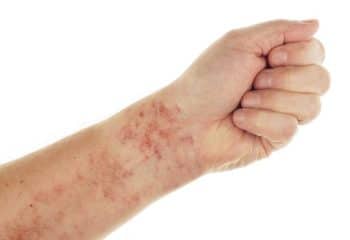
Schamberg’s illness (commonly called, “purpura pigmentosa progressiva” (PPP), “Schamberg’s purpura”, and “progressive pigmentary dermatosis of Schamberg”) is a persistent skin discoloration that affects persons of all ages, generally affecting the feet, legs, or thighs or a combination of these areas.[mfn]https://en.wikipedia.org/wiki/Schamberg_disease[/mfn]
It might happen as a single event, or it could spread over time. Males are the most affected. Jay Frank Schamberg, who reported it in 1901, is credited with its name. There is no known treatment for this illness, although it is not a deadly condition and is mostly of aesthetic significance, it may create reasonable psychological anxiety since it can arise so abruptly, so widely, and because it typically leaves lasting discoloration of the skin.
Itching caused by skin lesions may be relieved by administering cortisone cream. The cortisone cream simply alleviates irritation and does not enhance skin discoloration. Schamberg’s illness generates no additional symptoms aside from skin darkening and itching.
The illness is characterized by inflammation of the capillaries at the skin’s surface, which leads to red blood cell leakage into surrounding tissues. As red blood cells degrade and are mainly absorbed, part of the iron produced by red blood cells lingers in the skin, giving it a rusty look. Typically, the reason for this capillary irritation is unclear.
Watch the video for more details on this disease:
The Symptoms of Schamberg Disease (SD)
Lesions on the lower extremities are the most common, although they may develop anywhere on the human body, such as the hands, arms, chest, as well as the neck. They may fluctuate in quantity and erupt in large quantities.
They are made up of uneven patches of brown or orange pigmentation with “cayenne pepper” specks that form inside and around previous lesions. There are normally no symptoms, but there could be little itching, but no discomfort. The explosion might last for several years. The eruption pattern shifts, with modest expansion and typically some clearance of the underlying lesions.
Schamberg’s disease, also known as progressive pigmented purpuric dermatosis[mfn]Tristani-Firouzi P, Meadows KP, Vanderhooft S. Pigmented purpuric eruptions of childhood: a series of cases and review of literature. Pediatr Dermatol. 2001 Jul-Aug;18(4):299-304. [PubMed][/mfn], is a persistent skin discoloration that often affects the legs and progresses slowly. This condition is more frequent in men and may strike at any age, beginning in infancy. This illness is seen all over the globe and has no connection with race or ethnicity.
The Etiology or Cause of Schamberg Disease
The exact cause of Schamberg’s disease is not known. It is caused by extravasation of blood vessels particularly capillaries which allow red blood cells to get deposited into the skin which then releases their iron from hemoglobin. This iron causes a rust color accounting for the orange or brown tint of the rash.
The exact cause of capillary inflammation is unknown and can be multifactorial. Potential contributors in the etiology can be:
- Gravitational dependency
- Alcohol intake
- Drugs such as acetaminophen, aspirin, adalin, amlodipine, carbromal, chlordiazepoxide, glipizide, glybuzole, hydralazine, meprobamate, nitroglycerin, persantin, reserpine, thiamine, interferon-alfa, injection medroxyprogesterone acetate, topical fluorouracil, and sildenafil
- Genetic causes, as cases are seen in family members
- Hepatitis B antigenemia
- Dysfunctional immune system
- Idiopathic
The Mechanism of Action of Schamberg Disease
Schamberg disease is a skin ailment that produces pigmentation of the lower limbs. It mainly affects the lower limbs and very rarely elsewhere. This disorder is caused by leaking blood vessels located near the skin’s surface.
The origin of the leaking capillaries is unknown. When red blood cells leave the blood arteries, they wind up near to the skin’s surface, where they split apart, liberating hemoglobin, which then breaks down, releasing iron. (Iron is a component of hemoglobin that allows it to transport O2 from the lungs to cells, and carbon dioxide from cells to the lungs.)
The iron that is released into the skin is tied together into a complex compound called hemosiderin, which produces skin coloring.
Diagnosis of Schamberg disease
A dermatologist can typically identify if the lesions are caused by Schamberg’s disease based on a thorough history, the findings of a visual assessment, and the results of relevant laboratory tests.
Only a healthcare expert can accurately diagnose Schamberg’s illness. The ailment is frequently easily identified by a skilled skin expert, like a dermatologist, since the outward aspect of the lesions upon the skin itself usually implies that the cause is Schamberg’s disease. While evaluating medical history is helpful for diagnosing this ailment, a physical examination of the skin is also required.
A full blood count and other blood tests are often ordered by doctors to check that the lesions are just not triggered by other skin disorders or infections. Typically, blood test findings are normal.
They are generally used to rule out some other bleeding conditions that might produce purpura. Because Schamberg’s illness is frequently asymptomatic beyond the obvious lesions, further testing is normally recommended.
Additional tests might help with diagnosis. A skin biopsy may be performed to diagnose capillaritis of dermal veins. Capillaritis, also known as pigmented purpura, is a skin disorder characterized by brown-reddish spots on the skin produced by leaky capillaries.
Such skin samples are taken to a pathology laboratory for assessment, in which each biopsy is examined under a microscope. A skin specialist may also do a dermatoscopy.
Differential Diagnosis of Schamberg Disease (SD)
Differential diagnosis should be made with other cutaneous lesions that may present with petechiae, purpura, or localized hyperpigmentation related to hemosiderin deposition such as other DPPs.
Purpura annularis telangiectodes (Majocci disease), is characterized by annular, purpuric lesions[mfn]Zvulunov A, Avinoach I, Hatskelzon L, Halevy S. Pigmented purpuric dermatosis (Schamberg’s purpura) in an infant. Dermatol Online J. 1999 May;5(1):2. [PubMed][/mfn] and erythematous punctate lesions, and central clearing with slight atrophy.
Touraine, a variant of Majocci’s Disease, exhibits a purpura telangiectatic arciform, with fewer lesions, larger, and irregularly arciform.
Pigmented purpuric dermatosis of Gougerot and Blum is characterized by red-brown lichenoid papules that tend to fuse in plaques in older men
Eczematoid-like purpura of Doucas and Kapetanakis is usually bilateral, intensely itchy, and characteristically has eczematous features. Mild lichenification could be present and has a fluctuation course with spontaneous improvement occasionally.
Stasis dermatitis exhibits eczematous patches that progress to red-brown or brownish-colored irregular patches, associated varicosities, and leg edema, although both entities could coexist.
Leukocytoclastic vasculitis hemorrhagic bullae and brown pigmentation consistent with hemosiderin deposits, the palpable nature of the lesions, and the histopathology report differentiate it from SD.
Non-accidental injuries exhibit a purpuric patch that evolves and resolves in a few weeks.
Mycosis fungoides can be challenging to distinguish from SD, histopathology detection in the epidermis of large groups of lymphocytes, or many lymphocytes in the spinous layer favor mycosis fungoides.
Scurvy purpuric lesions could be confused, other features in scurvy such as perifollicular purpura, coiled hairs, bleeding gums, and dietary history of reduced vitamin C intake support scurvy.
Drug hypersensitivity reactions due to rituximab, carbamazepine, meprobamate, bufexamac, chlordiazepoxide, furosemide, nitroglycerin, vitamin B-1, or medroxyprogesterone acetate.
Treatment/Management of Schamberg Disease (SD)
There is no treatment for Schamberg’s illness, but this ailment is neither life-threatening nor a serious health problem. The most frequent difficulties that patients may confront is the darkening of the epidermis and, sometimes, itching. A cortisone cream may help alleviate itching.
Colchicine medication has only been utilized to prevent recurrence in extremely severe or worrying situations. Some doctors advise patients to take a vitamin C pill to boost collagen formation, but this has not been demonstrated to be effective. Persons should avoid re-exposure to known triggers.
For example, people suspected of being sensitive to foods containing artificial colors or preservatives must avoid foods containing such substances. This is because certain individuals are susceptible to these substances, and when they are exposed to them again, the body develops an inflammatory response, causing additional capillary inflammation and red blood cell leak.
Several research investigations have shown that the use of aminaphtone, a medication, may regulate Schamberg’s illness and minimize the number of lesions. This medication helps minimize capillary fragility and red blood cell leaking.
A 2014 research published in the Journal of the German Society of Dermatology finds that oral rutoside and ascorbic acid may be an effective and well-tolerated therapy for PPPD, with early treatment recommended for the best clinical result.
Many topical and systemic therapy for Schamberg disease has been attempted with varying degrees of success. A case study published in 2012 details the treatment of five individuals with Schamberg’s disease of the lower limbs with Advanced Fluorescence Technology (AFT) pulsed light with excellent outcomes.
Schamberg disease is still considered idiopathic. Without an established therapy, treatment is sometimes ineffective, and recurrences are not uncommon. It is not life-threatening or causes any major health concerns. Reassurance about the chronic and benign nature of the disease is required, and residual pigmentation could last for years.
First-line interventions are nonpharmacologic interventions and topical steroids. Various non-drug strategies are aimed at eliminating or reducing potential contributing factors such as discontinuing or changing the offending medication, avoiding food preservatives and artificial coloring agents, and wearing support stockings to counteract abnormal vein function.
The itching will improve with moisturizing, oral antihistamines, and topical steroids, such as cortisone or betamethasone, may be used. Topical steroids decrease inflammation by suppressing the migration of polymorphonuclear leukocytes and reversing capillary permeability. The use of anti-inflammatory drugs is used to treat skin diseases by immune mediation.
Second-line intervention: Pentoxifylline, a methylxanthine derivative, acts by various mechanisms.
- Potent rheological and anti-inflammatories properties.
- Immunomodulatory action by modifying cytokine profile and anti-fibroblastic action.
- A decrease in the expression of ICAM-I on endothelial cells of blood vessels that leads to decreased exudation of inflammatory cells from capillaries into the surrounding perivascular tissue.
- Inhibits synthesis and release of TNF-a, which also reduces the extravasation of blood from the capillaries.
Different clinical trials reported a clinical improvement from 2-3 weeks until six months, with doses ranging from 100-400 mg three times a day.
Phototherapy has been shown to be effective in a few case reports. Most of these were resistant to other therapies. Narrowband ultraviolet B therapy-induced immunomodulation by suppression of the interleukin-2 production and altering the T-cells activity.
It was used in two children and one adult two-three times a week for 10-20 treatments with improvement and without recurrence during the follow-up. Although it was effective in an adult, the treatment should be continued for a long period.
PUVA phototherapy diminished the CD4+ and CD1a+ cells and the adhesion molecule receptor has proved to be effective in eight patients. Intense pulse laser (IPL) acts through the absorption by the hemoglobin in the vessels generating thermal damage.
The Advanced Fluorescence Technology, a new generation of IPL, selectively targets hemosiderin within macrophages and hemoglobin within extravasated erythrocytes shown to be effective in 5 patients.
Multiple other therapies have been utilized for SD, although only a few of them have been effective. Ascorbic acid and bioflavonoids have additive antioxidative properties that wield an angio-protective and anti-inflammatory effect. It also decreases the permeability of endothelial cells and reduces capillary permeability and fragility by increasing their resistance.
Three patients were treated with 500 mg bid and 50 mg bid, respectively, with clinical improvement at four weeks. Colchicine 0.5 g bid has been used with the improvement from the first week to complete clearance by the four months. Aminaphtone helps reduce capillary fragility, and red blood cell leakage reported improvement with 75mg bid for one month without recurrence for one year after suspension.
Griseofulvin could have an immunomodulatory activity improving the SD at a dose of 500-750 mg since the first week. Variable results are found with other drugs, also as oral cyclosporine, calcineurin-inhibitors, and methotrexate.
Complications of Schamberg Disease (SD)
In general, SD is a benign condition, although it can cause worsening and recurrent chronic skin lesions, resistant to treatment.
There are infrequent reports of patients with SD that developed mycosis fungoides presented as SD. Clinical and histopathological properties shared some similarities. Although it is rare to develop mycosis fungoides after an initial diagnosis of SD, this could be suspected when it has a long-lasting course (>1 year), and follow-up could be made every year.
Emotional stress and psychological trauma can come due to the longstanding pigmentation in the skin leading to depression and anxiety in some patients.
The Prognosis
The course of the condition is typically chronic, with numerous exacerbations and remissions. Lesions could persist or extend with time and spontaneous resolution also may occur in a period ranging from months to years. Ratnam et al reported in a series of cases in which 62% of the patients cleared entirely while 38% remained stable or experienced worsening of their symptoms.
A patient with Schamberg’s disease can live a normal and healthy life. Since there is no proven cure for this condition, the patient will have to endure the lesions on his or her skin. With appropriate treatments, the condition may get better.
Although the skin lesions are not life-threatening, they may cause a cosmetic concern for some individuals. Skin lesions may cause psychological discomfort, and patients may require reassurance to help with stress and anxiety.
There are a few rare cases of T-cell lymphoma that have developed from Schamberg’s disease. This is not a cause for concern, since the risk factors associated with Schamberg’s disease are relatively low.
All right, guys, that is it for now for Schamburg disease. I hope Healthsoothe answered any questions you had concerning the schamberg disease.
Feel free to contact us at [email protected] if you have further questions to ask or if there’s anything you want to contribute or correct to this article. And don’t worry, Healthsoothe doesn’t bite.
You can always check our FAQs section below to know more about schamberg disease. And always remember that Healthsoothe is one of the best health sites out there that genuinely cares for you. So, anytime, you need trustworthy answers to any of your health-related questions, come straight to us, and we will solve your problem(s) for you.
[bwla_faq faq_topics=”frequently-asked-questions-concerning-schamburg-disease” sbox=”1″ paginate=”1″ pag_limit=”5″ list=”1″ /]
