The reasons for tooth extraction include impacted wisdom tooth or a tooth that is dead and too badly damaged beyond repair. Tooth extraction is less painful than before under local anesthesia and most pain disappears within a week.
However, in some cases, if you have your tooth removed you may experience little or no discomfort and only minor bleeding.
The main goal of a dentist is to preserve your natural teeth and keep them healthy for as long as possible. There are times when it is of best interest (or your child’s) to have a tooth extracted (removed). This could be the case for a variety of reasons for tooth extraction:
Whatever the reasons, tooth extraction is more often than not a very routine procedure. However, minor surgery depends on where the tooth to be extracted and where it is located in your mouth, and what its roots are like.
Still, tooth extraction is nothing to be feared when done by an experienced dentist. You should also be aware that a tooth is not rigidly fixed in its surrounding bone, though that’s how some may picture it.
In fact, it is attached to the bone via a network of fibers that form what’s known as the periodontal ligament. By carefully manipulating the tooth, these fibers can be detached and the tooth freed without much trouble.
1. Reasons for tooth extraction (Wisdom Teeth)
Today, we remove more wisdom teeth than any other teeth. Common problems with wisdom teeth (impacted teeth) include pericoronitis, caries, and inflammation of the dental pulp.
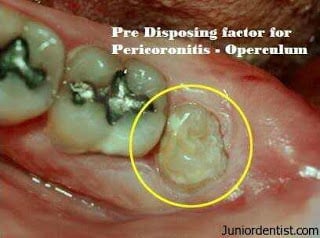
PERICORONITIS

Pericoronitis is the swelling of the tissue that surrounds you partially erupted wisdom tooth (last teeth). It is a very common dental problem this day and usually affects young people.
About 95% of pericoronitis cases occur in lower wisdom teeth. As wisdom teeth are not important for maintaining a correct occlusion, or bite, they are often extracted.
Pericoronitis is the most common wisdom tooth problem among young adult. It occurs as a result of microbes and food that get trapped in the space between a partially erupted wisdom tooth (right edge of the picture) and gum.
Minor symptoms of acute pericoronitis are swollen gum tissue around your wisdom tooth, pain and a bad taste in your mouth. More serious symptoms that you need to see your doctor for immediate treatment include fever, wisdom tooth-related abscess, and difficulty opening your mouth because of swelling.
Pericoronitis is the basic reasons for tooth extraction usually develops when your wisdom teeth start to erupt. It is rare in people over 30 years of age.
CARIES, PULPITIS AND TOOTH ROOT INFECTION
Caries, or tooth decay, is a common problem, particularly with wisdom teeth. If left untreated, caries can lead to pulpitis, which is an inflammation of the dental pulp.
Pulpitis can cause throbbing pain in the tooth. It can reach the tooth pulp and lead to tooth root infection, also known as apical periodontitis if left untreated. Tooth root infection is a common reason for tooth extraction.

orthodontic and prosthetic treatments
Orthodontics Treatment – Teeth are sometimes extracted when there are too many of them for the size of the dental arches (jaws), a situation known as crowding or supernumerary teeth. After an adequate amount of space is opened up through the extraction of one or more teeth, the remaining teeth can be aligned properly.
The teeth most frequently removed for orthodontic reasons are the first premolars, which are right next to the canines. as well as the treatment of cysts or tumors in the jaw area. Although they are less common reasons for tooth extraction.
Baby Teeth
These are other reasons for tooth extraction if is out of position or not lost in the right sequence, the permanent tooth underneath it might not erupt normally. In this case, removing the baby tooth could prevent a need for orthodontic treatment later on.
PERIODONTITIS IS ONE OF THE REASONS FOR TOOTH EXTRACTION
Periodontitis damages the tissue and bone that support your tooth and can cause the tooth to become weaken and loose. Removing and, if necessary, replacing your tooth with a dental implant can be the only reasonable treatment option for you.

Other Reason to remove your teeth
- Aesthetic reason.
- Damage tooth.
- Accident.
- Root fractures and cracks.
- Avulsed tooth.
If your dentist notices a tooth with a severe infection, it may need to be removed proactively, particularly before starting a strong medication or undergoing surgery.
If you are diagnosed with cancer or rheumatoid arthritis, your medications may weaken your body immune system, and even minor tooth infections can then quickly spread and cause severe health problems.
For your surgical treatments to succeed and for you to recover, your blood must be free of bacteria. Bacteria are found in damaged teeth, so your mouth and teeth should be checked and any damaged teeth extracted before starting a strong medication or undergoing a challenging surgery.
If you are in certain professions (such as divers, pilots, and soldiers) the risk of teeth infections is reduced by removing teeth that may cause the problem. Root fracture and cracks are the other reasons for tooth extraction.
Alternatives to tooth extraction
If your tooth’s pulp or root is infected, your dentist may perform tooth extraction or root canal treatment. You can also refuse treatment if you want or postpone it and leave the infection untreated.
It is assumed that the infection can be treated with root canal treatment.
NO TREATMENT
- Free of charge
- Risk of infection in the head and neck area
- Infection doesn’t go away without treatment
- Easier and cheaper to treat when done on time
TOOTH EXTRACTION
- Quick treatment
- Good prognosis
- Tooth is lost
- Teeth other than wisdom teeth may need to be replaced with dental implants, which is expensive
ROOT CANAL TREATMENT
- Usually good prognosis
- Better than dental implants if performed properly
- Requires multiple visits
Treating infected teeth with root canal treatment may not be possible if you have root fraction or advanced infection.
Moreover, root canal treatment is not recommended when a tooth is very damaged and can not be repaired. Teeth extraction can then be the best treatment option.
What is the Process of Extracting a Tooth?
- The first step is to do an oral diagnosis and have a radiographic (x-ray) examination to assess the position of your tooth roots and the condition of your surrounding bone. This will allow any possible complications that are expected to happen.
A thorough medical and history taking in medicine are also conducted by your dentist. This is to ensure all procedure done for you in the clinics is less painful with no discomfort, and no complications.
- Tooth extraction is usually carried out with local anesthesia, without you feeling when the teeth are been removed, with the surrounding bone and gum tissues.
Additional sedatives might also be used, including oral sedatives (taken in pill form), nitrous oxide (which is inhaled) and/or conscious sedation, which is given intravenously (into a vein).
The is usually required if you have more complicated (or multiple) tooth extractions. By the time the sedation medication has worn off, you won’t even be aware that the surgery was done.
- Once you have been appropriately anesthetized, the gum tissue at the extraction site may need to be opened if the tooth is impacted ( For example the last molar impacted tooth or wisdom tooth). The tooth itself will then be gently removed.
As your tooth is being removed, steps are taken by your dentist to ensure the bone that surrounds it isn’t damaged. Sometimes, in the process of removing a tooth, a small amount of lab-processed bone-grafting material is placed into the socket to help preserve the bone volume there.
This is particularly important when the extraction is going to be followed at some point by the placement of a dental implant, which needs to fuse to existing bone, or orthodontics, which gently moves teeth through bone.
What to expect after tooth extraction?
Immediately after your tooth is extracted, the socket will be covered with sterile gauze; gentle pressure will be applied for 10-20 minutes to control any bleeding from the extraction site. Small sutures (stitches) might also be used for this purpose. Your dentist or dental nurse we also recommend resting with your head elevated on pillows to help the clotting process.
It’s normal to experience some mild to moderate post-operative discomfort and/or swelling. Taking non-steroidal, anti-inflammatory drugs such as ibuprofen and/or aspirin the day of surgery should control most symptoms. Antibiotics may also be prescribed to ensure infection-free healing.
Smoking, vigorous brushing and rinsing, and drinking liquids through straws are discouraged during the post-operative period because they hinder healing and may cause the wound to open. Also, be careful when brushing or putting anything in your mouth until your healing is complete.
Cold compresses applied to the outside cheek near the extraction area can help reduce any swelling and promote faster healing. Eating softer foods, and rinsing the mouth with warm salt water a few days after the procedure until you feel more comfortable can also be helpful.
Be sure to follow the post-operative instructions you are given by your dental nurse, as each case is a little different. Within a few days, all should be back to normal.
Tooth extraction cost
The cost of tooth extraction is determined by how difficult it may seem. Upper wisdom teeth are usually easier to remove than lower wisdom teeth.
Dentists who specialize in surgeries of the mouth (oral and maxillofacial surgery) charge around 30% more than other dentists.
SIMPLE TOOTH EXTRACTION
- Front, premolar or fully erupted wisdom tooth extraction
- Procedure code EBA00
CHALLENGING TOOTH EXTRACTION
- Challenging front, premolar, molar or wisdom tooth extraction
- Procedure code EBA05
SURGICAL TOOTH EXTRACTION
- Extracting, for example, a molar or wisdom tooth that is only partially erupted or that is difficult to extract for some other reason
- Procedure code EBA10 or EBA12
Wisdom tooth pain is the most common reasons for tooth extraction for young adults. If you feel pain seek emergency dental care. Your dentist will examine your tooth, the gums around it and the neighboring teeth.
Your dentist may also examine other wisdom teeth and the lymph nodes in the neck, looking for occlusion and swelling inside and outside the mouth.
X-rays are often used to examine wisdom teeth and to detect any infections in your teeth, roots and surrounding tissues. X-rays also show the shape and position of your roots in the jawbone.
References
Mayo Foundation for Medical Education and Research (MFMER)
Family dental care/extractions/
Avila G, Galindo-Moreno P, Soehren S et al. A novel decision-making process for tooth retention or extraction. J Periodontol 2009;80:476-491.
Bailey E, Worthington HV, van Wijk A et al. Ibuprofen and/or paracetamol (acetaminophen) for pain relief after surgical removal of lower wisdom teeth. Cochrane Database Syst Rev 2013;12:CD004624.
Dicus-Brookers C, Partrick M, Blakey GH 3rd et al. Removal of symptomatic third molars may improve the periodontal status of remaining dentition. J Oral Maxillofac Surg 2013;71:1639-1646.
Klein OD, Oberoi S, Huysseune A et al. Developmental disorders of the dentition: An update. Am J Med Genet C Semin Med Genet 2013;163:318-332.
Lodi G, Figini L, Sardella A et al. Antibiotics to prevent complications following tooth extractions. Cochrane Database Syst Rev 2012;11:CD003811.
Muhonen A, Ventä I, Ylipaavalniemi P. Factors predisposing to postoperative complications related to wisdom tooth surgery among university students. J Am Coll Health 1997;46:39-42.
Nitzan DW, Tal O, Sela MN et al. Pericoronitis: a reappraisal of its clinical and microbiologic aspects. J Oral Maxillofac Surg 1985;43:510-516.
Pogrel MA. What is the effect of timing of removal on the incidence and severity of complications? J Oral Maxillofac Surg 2012;70:S37-40.
Suomalaisen Lääkäriseuran Duodecimin ja Suomen Hammaslääkäriseura Apollonia ry:n asettama työryhmä. Viisaudenhammas. Käypä hoito -suositus. Julkaistu: 18.08.2014