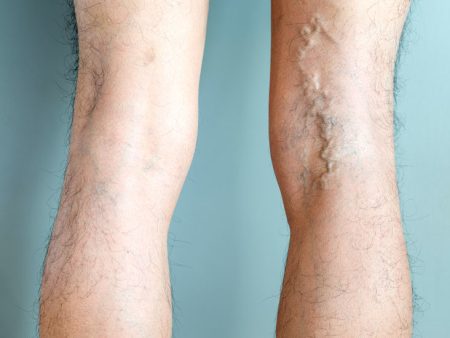
When a girl is born with an abnormally small uterus (womb), the condition is known as a hypoplastic uterus, also known as uterine hypoplasia, small uterus, or underdeveloped uterus. A congenital condition, the hypoplastic uterus is one that exists from birth.
The hypoplastic uterus can be characterized by
- Simple uterine hypoplasia: a small uterus with a normal shape.
- An extended uterus with a normal fundus is called elongated uterine hypoplasia.
- Malformative uterine hypoplasia: a uterus with an unusual shape
Hypoplastic uterus causes
When a fetus's uterus does not fully develop, hypoplastic uterus results. It is unknown what is causing this abnormal foetal development.
The Mayer-Rokitansky-Küster-Hauser syndrome, a disorder in which the girl's uterus and vagina are absent or underdeveloped as a result of an early arrest in Mullerian duct development, among other abnormalities, may have hypoplastic uterus as one of its symptoms.
In addition to having a 46 XX karyotype, women with the Mayer-Rokitansky-Kuster-Hauser (MRKH) syndrome also have normal female secondary sex characteristics, normal ovarian functions, and an underdeveloped vagina.
The prevalence is 1 per 400–10,000 live births of females. MRKH syndrome is a type A and type B atypical Mullerian duct anomaly that is classified as a class one anomaly. Patients with type A syndrome have normal fallopian tubes and symmetric muscular buds.
Patients with type B have asymmetrical muscle buds and abnormal fallopian tubes, and they could also have other congenital anomalies like renal, skeletal, hearing, cardiac, and ocular anomalies.
The likelihood of a genetic connection is suggested by the familial distribution of these cases. A mutation of the WNT4 gene, a developmental gene that controls growth and differentiation during embryogenesis, is one candidate among the few genes that have been implicated in causation.
Gonadal dysgenesis is the most frequent factor, followed by Mayer-Rokitansky-Kuster-Hauser (MRKH) syndrome, in the failure to start menstruating at puberty (primary amenorrhea).
Perrault syndrome 7 and Swyer syndrome may both be connected to the hypoplastic uterus.
Swyer syndrome
Pure 46XY gonadal dysgenesis, another name for Swyer syndrome, is a disorder that impacts sexual development. Chromosomes typically control how a person develops sexually; however, in Swyer syndrome, sexual development differs from the afflicted person's chromosomal makeup.
46 chromosomes are typically found in each human cell. The X and Y chromosomes, two of the 46 chromosomes, are referred to as the sex chromosomes because they influence whether a person would exhibit male or female sex traits.
Boys and men normally have one X chromosome and one Y chromosome, whereas girls and women typically have two X chromosomes (46, XX karyotype) (46, XY karyotype).
People with Swyer syndrome (46XY gonadal dysgenesis) have female reproductive organs because they have one X and one Y chromosome in each cell, which is a pattern generally observed in boys and men.
Swyer syndrome patients have normal external genitalia for women. The gonads (ovaries or testes) are not functioning in afflicted people; instead, they are immature tissue clumps known as streak gonads.
The uterus and fallopian tubes are both properly formed. The remaining gonad tissue is often malignant since the gonads did not grow properly, thus it is typically removed surgically at a young age.
Swyer syndrome patients often identify as feminine and were reared as females. Affected people often start hormone replacement treatment in adolescence to induce menstruation and the development of female secondary sex traits including breast expansion and uterine growth since they do not have functioning ovaries.
Additionally, hormone replacement treatment lowers the possibility of decreased bone density (osteopenia and osteoporosis).
Women who have this illness are unable to develop eggs (ova), but they may be able to conceive using an egg or embryo that has been given.
Isolated Swyer syndrome refers to instances of Swyer syndrome, which often exclusively impact sexual development. Nevertheless, depending on the underlying genetic aetiology, Swyer syndrome may also develop in conjunction with other medical diseases like neuropathy or as a component of a syndrome like campomelic dysplasia, which results in severe skeletal anomalies.
Perrault syndrome
Males and females with Perrault syndrome exhibit varied patterns of signs and symptoms. Perrault syndrome is an uncommon hereditary disorder. Hearing loss, specifically sensorineural hearing loss in females and deafness alone in affected males, is a key symptom of Perrault syndrome 7.
Females who are affected also have ovarian abnormalities. Some males and females who are affected both experience neurological issues.
Sensorineural hearing loss, also known as changes in the inner ear, is the cause of the hearing issues in Perrault syndrome. The condition, which typically affects both ears, can exist from birth or develop in a child's early years. Unless the hearing is totally lost at birth, hearing issues get worse with time.
Despite having normal external genitalia, females with Perrault syndrome have abnormal or absent ovaries (ovarian dysgenesis). Girls who are severely affected do not start menstruating by the age of 16 (primary amenorrhea), and the majority never do.
Primary ovarian insufficiency, which affects less severely affected women, results in an early loss of ovarian function; although menstruation starts in adolescence, it gradually becomes less regular and eventually stops before the age of 40.
Women who have Perrault syndrome might have trouble getting pregnant or won't be able to have biological children.
Intellectual disability, ataxia, loss of sensation, and weakness in the limbs are just a few of the neurological issues that people with Perrault syndrome may experience. But not everyone who has this condition experiences neurological issues.
Hypoplastic uterus symptoms
Hypoplastic uterus symptoms
- Failure to start having periods at puberty (primary amenorrhea)
- Abdominal pain
- A small or no vaginal opening
- Infertility
Hypoplastic uterus treatment
The patient's symptoms and the underlying cause of her hypoplastic uterus will determine the best course of treatment.
Treatment for Mayer Rokitansky Kuster-Hauser syndrome focuses on the distinctive symptoms that are noticeable in each patient.
The coordinated efforts of a group of specialists may be necessary during treatment. Paediatricians or internists, gynaecologists, kidney specialists (nephrologists), endocrinologists, orthopaedic surgeons, plastic surgeons, physical therapists, psychiatrists, and other medical professionals might need to collaborate to ensure a comprehensive approach to treatment, depending on the affected person's age at diagnosis.
It is recommended that women with Mayer Rokitansky Kuster-Hauser syndrome seek counselling both before and after receiving a diagnosis because these conditions are prone to anxiety and severe psychological distress. Affected females and their families are advised to seek professional counselling and psychological support, as well as to participate in support groups.
The Mayer Rokitansky Kuster-Hauser syndrome will typically be treated with appropriate management of the physical findings connected to it as well as psychological support for the emotional problems that frequently go along with the diagnosis.
Making a neovagina for sexual activity is the mainstay of vaginal aplasia treatment. When women are ready to engage in sexual activity and are emotionally mature, this should be proposed to them.
There are two types of treatment: nonsurgical and surgical. The first-line treatment involves nonsurgical methods.
Specially made plastic tubes known as vaginal dilators are used to help create or enlarge a vagina. Franck's dilator method is the most popular technique. With this technique, a doctor (and then the patient) applies a vaginal dilator, gradually stretching and widening the vagina.
It is possible to carry on with this daily routine for up to six weeks or several months.
It might be necessary to undergo plastic surgery to make an artificial vagina. There is no universal agreement on the best surgical technique among the many different ones that may be employed. In order to increase their chances of success, female patients who have surgery to create an artificial vagina will probably need to use vaginal dilators after the procedure.
Conclusion:
Since the genitalia on the outside seems normal, the hypoplastic uterus is frequently not discovered until a girl reaches puberty, when she stops menstruating and consults her doctor.
Starting with a comprehensive medical history and physical examination that includes a pelvic exam, a hypoplastic uterus is diagnosed.
My name is Wisdom Bassey, I’m a blog content writer and graphic designer who provides support and services for brands and different companies. I’m young and versatile, A tech enthusiast. I carry out deep research on every topic I choose to write about. You can reach me through my social media handles, I’m always available and ready to connect.