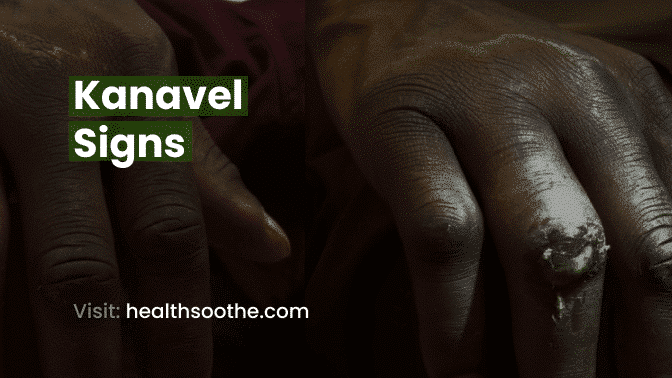
The clinical symptom known as Kanavel’s sign is seen in people who have flexor tenosynovitis, a dangerous illness that may quickly result in the loss of function of the afflicted finger. The cardinal signs of Kanavel. a variety of diagnoses of inflammation of the flexor tendon sheath.
Hand infections are a widespread issue in society and are associated with high morbidity. To avoid lifelong handicaps, deep hand infections such as [mfn]flexor sheath infections[/mfn] are surgical emergencies that need an urgent referral.
A flexor sheath infection misdiagnosis may result in severe stiffness, [mfn]deformity[/mfn], or amputation of the affected digit.
An unusual case of a 22-year-old with a long history of swelling and pain in the right middle finger is presented in this article. Despite the slightly atypical history, the examination revealed the Kanavel cardinal signs of tendon sheath infection.
With a frequency ranging from 2.5% to 9.4% of hand infections, flexor sheath infections, also known as infected tenosynovitis, are very frequent hand infections. 3 Flexor sheath infections may have severe, even fatal, effects if undiagnosed.
The flexor digitorum profundus and flexor digitorum superficialis are enclosed by closed, continuous synovial sheaths called digital flexor sheaths. Flexor sheath infections can be brought on by haematogenous spread, contiguous spread from nearby tissues, or direct inoculation as a result of trauma.
Animal bites, puncture wounds, IV drug use, and wounds from exposure to freshwater or saltwater are some common injuries. If such injuries are accompanied by extreme tenderness, flexor tenosynovitis should be strongly suspected.
Exudative fluid within the tendon sheath is the first sign of a flexor sheath infection, which is followed by the development of purulent fluid. In the synovial sheath, bacterial overgrowth causes an increase in fluid and pressure, which causes ischaemia and septic necrosis of the tendon sheath and the structures nearby.
Osteomyelitis, necrotizing fasciitis, and soft tissue necrosis are possible complications if untreated. The four Kanavel signs, also known as the cardinal signs of flexor tenosynovitis, are as follows:
- a fine soreness across the sheath and just inside the sheath;
- the finger is in a relaxed, extended position;
- severe discomfort with finger extension especially pronounced at the proximal end; and
- an all-over fusiform swelling of the finger.
When all four Kanavel symptoms are present, flexor tenosynovitis is diagnosed with high sensitivity (91–97%). 6 The first symptom is often discomfort during passive extension3, and the second symptom is soreness along the flexor sheath, which may indicate that the infection is progressing closer to the area of sensitivity. Contrary to the majority of serious illnesses, fever is seldom absent (approximately 17%). 3
Elevation to minimise swelling and an immediate referral to the neighbourhood hand surgery department are the two methods used to treat suspected flexor tenosynovitis in the general population. Broad-spectrum antibiotic medication and prompt surgery to debride tissues and irrigate the tendon sheath are part of inpatient care. 3
This patient’s history of RMF discomfort and edema was unusual. His GP gave him a comprehensive examination, which showed the Kanavel symptoms of flexor sheath infection. Although the diagnosis was originally unclear, the thorough referral elevated the duty-hand consultant’s concerns, leading him to ask for rapid surgical evaluation and treatment.
In conclusion, flexor sheath infections are a serious hand ailment that all general practitioners (GPs) should be aware of, as well as the possible repercussions of ignoring these infections. Even if the history may not always be typical, if clinical symptoms are found during the examination, such as the Kanavel signs, an immediate same-day referral to a hand service should be taken into consideration.
Read Also: What are the 5 Signs of Appendicitis?
How is flexor tenosynovitis treated?
Naturally, the cause of the inflammation will have no bearing on how to treat tenosynovitis. For nonsuppurative flexor tenosynovitis, nonoperative therapy is commonly undertaken, although persistent cases may need surgical intervention.
However, infectious flexor tenosynovitis continues to be an orthopaedic emergency, and there is only a very little window of opportunity to try the nonoperative treatment. As a result, many surgeons advise early surgical drainage in all circumstances.
Can a flexor tendon heal without surgery?
You won’t be able to bend one or more fingers if your flexor tendons are injured. In addition to causing pain and swelling in your hand, tendon injury may also cause it. Damage to the extensor tendons may sometimes be addressed without surgery by wrapping the hand in stiff support known as a splint.
In order to detect the ends of the split tendon and suture them together during tendon repair, the surgeon may need to make an incision in your wrist, hand, or finger.
Extensor tendons are simpler to repair since they are easier to access. Extensor tendons may be repaired at an accident and emergency (A&E) department using a local anaesthetic to numb the injured region, depending on the kind of damage.
Because the flexor tendon system is more intricate, flexor tendon repairs are more difficult. A skilled plastic or orthopaedic surgeon with expertise in hand surgery is often required to perform flexor tendon repair in an operating room under either a general anaesthetic or a regional anaesthetic (where the whole arm is numbed).
The fact that the restored tendons will remain frail until the ends come together necessitates a prolonged time of recuperation (rehabilitation) after both forms of tendon surgery. It may take up to 3 months for the repaired tendon to recover its prior strength, depending on where the lesion occurred.
Using a hand splint during rehabilitation entails shielding your tendons from excessive use. After surgery, you’ll typically need to wear a hand splint for a few weeks.
Regular hand exercises are also necessary during your recovery to prevent the repaired tendons from adhering to the surrounding tissue and limiting your hand’s range of motion.
Your job will determine when you can go back to work. After 6 to 8 weeks, light activity can frequently be resumed, and after 10 to 12 weeks, heavy activity and sport.
Conclusion:
You should be able to use your finger or thumb after an extensor tendon repair, although you may not get complete mobility back. When the tendon is injured cleanly as opposed to being crushed or having its joints or bones damaged, the prognosis is often better
Due to their frequent exposure to greater strain than extensor tendons, flexor tendon injuries are often more severe. It’s fairly uncommon for some fingers to not fully recover their range of motion after a flexor tendon repair. The tendon repair will still provide better results than forgoing surgery, however.