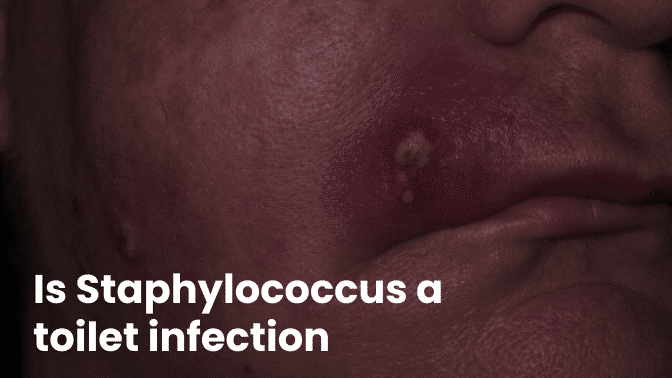
Staphylococcus is a type of bacteria that is commonly found on the skin and in the nasal passages of humans. While there are many different types of staphylococcus bacteria, the most common one that causes infections is called Staphylococcus aureus.
This bacteria can cause a wide range of infections, from mild skin infections to more serious illnesses like pneumonia and sepsis.
One of the questions that people often ask is whether staphylococcus is a toilet infection. The answer to this question is not straightforward, as there are many different ways that staphylococcus can be transmitted.
But, there is a chance that staphylococcus will be present in restrooms, and there are several steps you may do to lower your risk of becoming sick.
Staphylococcus may be discovered in a variety of locations, including on objects like toilet seats, door knobs, and tabletop surfaces. A person may spread staphylococcus bacteria to a surface by coming into touch with it while carrying the bacterium on their skin or in their nasal passages.
Read Also: Query: Can Yoni Pearls Cure Staphylococcus?
Symptoms
Symptoms of staphylococcus infection can vary depending on the type of infection and the severity of the infection. Some common symptoms include:
- Skin infections: Staphylococcus infections on the skin can cause redness, swelling, warmth, and pain at the site of the infection. They may also cause boils or pus-filled blisters.
- Food poisoning: If you consume food contaminated with staphylococcus bacteria, you may experience symptoms such as nausea, vomiting, stomach cramps, and diarrhoea.
- Respiratory infections: Staphylococcus bacteria can also cause respiratory infections like pneumonia. Symptoms of respiratory infection may include cough, chest pain, and difficulty breathing.
- Blood infections: In severe cases, staphylococcus can cause a bloodstream infection called sepsis. Symptoms of sepsis may include fever, chills, low blood pressure, and rapid breathing.
- Toxic shock syndrome: In rare cases, staphylococcus can cause toxic shock syndrome, a serious condition that can cause symptoms such as fever, rash, low blood pressure, and organ failure.
It’s important to seek medical attention if you experience any symptoms of a staphylococcus infection, as prompt treatment can help prevent complications.
What Causes Staphylococcus
Staphylococcus infections are caused by bacteria from the Staphylococcus genus, most commonly Staphylococcus aureus. These bacteria are commonly found on the skin and in the nasal passages of humans. Staphylococcus infections can be caused by:
- Direct contact: The bacteria can be spread through direct contact with infected skin or contaminated objects, such as towels or razors.
- Indirect contact: The bacteria can also be spread indirectly through contact with surfaces contaminated with the bacteria, such as door handles, furniture, or medical equipment.
- Food contamination: Staphylococcus bacteria can also contaminate food and cause food poisoning.
- Surgical site infections: Staphylococcus infections can occur after surgery when bacteria enter the body through an incision or wound.
- Catheter-associated infections: Staphylococcus bacteria can cause infections in patients with catheters or other medical devices.
- Hospital-acquired infections: Staphylococcus infections can be acquired in hospitals and other healthcare settings, where patients may be more susceptible to infections due to weakened immune systems or invasive medical procedures.
- Community-acquired infections: Staphylococcus infections can also be acquired in the community, such as in schools, gyms, and other public places.
To stop the spread of staphylococcus infections, it’s crucial to practise good hygiene, take measures, and wash your hands often. You should also avoid sharing personal belongings and seek medical assistance if you think you could be infected.
Diagnosis
Diagnosing a staphylococcus infection typically involves a combination of physical examination, medical history, and laboratory tests. Here are some common methods used to diagnose staphylococcus infections:
- Physical examination: A doctor will examine the affected area and look for signs of infection, such as redness, swelling, and warmth.
- Medical history: A doctor will ask about your symptoms, medical history, and recent activities to help determine the possible cause of the infection.
- Laboratory tests: A doctor may order laboratory tests to confirm the presence of staphylococcus bacteria, identify the specific type of bacteria, and determine the best course of treatment. These tests may include:
- Blood tests: Blood tests can detect signs of infection and help identify the specific bacteria causing the infection.
- Wound culture: A sample of tissue or fluid from the infected area is collected and tested to identify the bacteria causing the infection.
Treatment of Staphylococcus
The treatment of Staphylococcus infections depends on several factors, including the severity of the infection, the type of Staphylococcus bacteria involved, and the patient’s overall health.
- Antibiotics: Antibiotics are the primary treatment for Staphylococcus infections. The choice of antibiotic depends on the type of Staphylococcus bacteria involved and the sensitivity of the bacteria to various antibiotics. Methicillin-resistant Staphylococcus aureus (MRSA) is a strain of Staphylococcus that is resistant to many antibiotics, including methicillin and is often treated with vancomycin or other antibiotics.
- Incision and Drainage: For skin and soft tissue infections, incision and drainage may be necessary to remove pus and other infected material. This can help speed up the healing process and prevent the infection from spreading.
- Supportive Therapy: In addition to antibiotics, supportive therapy may be necessary to treat Staphylococcus infections. This can include pain management, fever management, and IV fluids to help maintain hydration.
- Prevention: Preventing Staphylococcus infections is also an important part of treatment. Good hand hygiene, keeping wounds clean and covered, and avoiding contact with infected individuals can all help reduce the risk of infection.
It is essential to keep in mind that a healthcare expert should be consulted for the correct diagnosis and treatment of Staphylococcus infections since improper antibiotic usage may lead to antibiotic resistance and other issues.
Conclusion
While staphylococcus can be present in toilet facilities, it is not necessarily a toilet infection. Staphylococcus can be found in many different environments, and there are many different ways that it can be transmitted.
By practising good hygiene and seeking medical attention if you think you may have an infection, you can reduce your risk of contracting staphylococcus and other bacterial infections.
[bwla_faq single=”1″ fpid=”35752″/]